Preventing Surgical Site Infection Post-Caesarean Birth
Published: 07 September 2021
Published: 07 September 2021

Surgical site infection (SSI) is a common complication of caesarean birth, occurring in up to 12% of all caesarean births globally (Shea & Soper 2019).
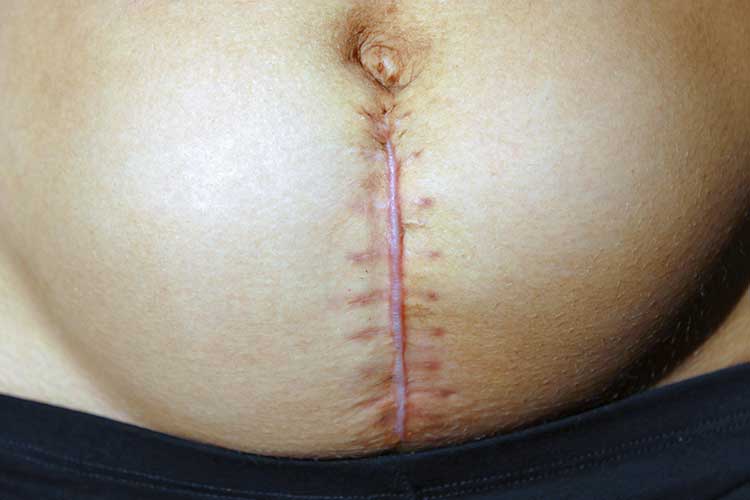
SSI typically presents between four and seven days post-delivery with erythema, discharge and induration of the surgical incision (Kawakita and Landy 2017).
The main causative organisms for SSI are Staphylococcus aureus, coagulase-negative staphylococci and Enterococcus spp. When wound infection develops within the first 48 hours, the causative microorganisms are usually groups A or B-haemolytic Streptococcus.
Not only does SSI cause distress for the mother and prolonged postnatal recovery, but it can also cause significant additional strains on staff time and hospital resources.
As the rate of caesarean birth continues to increase in developed countries, there is also a corresponding rise in the incidence of SSI (Baxter & Lymn 2015).
With sepsis being a potential cause of maternal mortality (AIHW 2020), wound care management is becoming an increasingly important area of concern for midwives. As Murphy (2013) points out, with 50% of women who have died from sepsis having had a caesarean birth, the question of what else can be done to prevent infection is arising.
The major risk factors for SSI include both maternal and operative factors.
Maternal factors include:
Surgical factors include:
(Kawakita & Landy 2017; Murphy 2013)
Along with these risk factors, it’s also thought that women are more likely to develop SSI if they actively laboured before delivery by caesarean birth (Murphy 2013).
Martin (2014) describes how the use of a safety checklist can provide a more structured approach to ensuring, for example, that antibiotics are offered pre-operatively. Other infection prevention strategies such as instructing women not to remove pubic hair in the month before the expected date of delivery, and general wound management education, are also important. Other effective interventions to decrease the risk of surgical site infection include:
(Kawakita & Landy 2017)
The National Institute for Health and Care Excellence (2021) suggests that no particular type of wound dressing is better than another at reducing the risk of SSI. Negative-pressure wound therapy should also be considered for women with a BMI of 35 kg/m2 or higher to reduce the risk of infection. General guidelines to prevent infection include:
(NICE 2021)
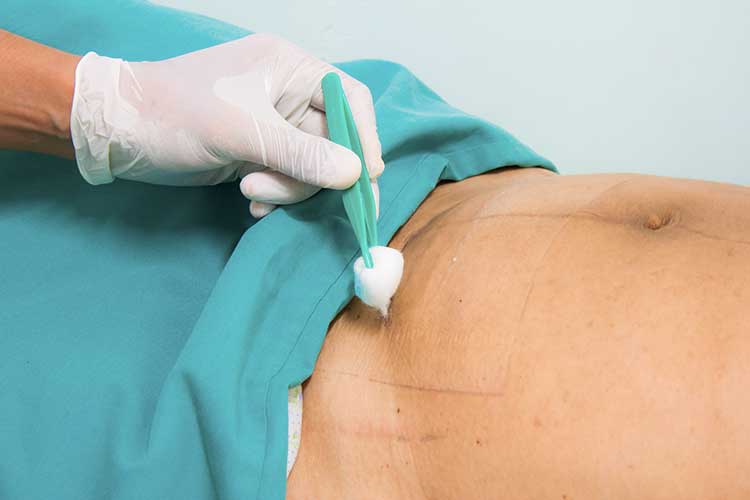
It can take two to six weeks for a caesarean birth wound to heal completely and in most cases, the wound dressing will be removed prior to discharge with the following self-care advice:
(Fox 2011)
Mothers should also be advised not to:
(Fox 2011)
If any of the following symptoms occur, mothers should also know who to contact for treatment and advice:
(Fox 2011)
Villers (2020) proposes that approximately 10% of women with a caesarean birth wound experience a complication, most commonly an infection that can cause significant disruption to their life during the postpartum period.
Villers (2020) also goes on to suggest that 39% of postpartum hospital readmissions are due to SSI. However, they also note that this number could be even higher in reality, as most studies do not capture the number of women diagnosed with SSI who are treated as an outpatient. This makes the true cost of complications hard to assess, and to date, there is no reliable published data on the true impact that wound complications have on maternal postpartum recovery.
Wound care is now an integral part of postnatal care, and with this comes the need for specific training packages to help maternity staff keep up-to-date with the latest research into wound care products (Baxter and Lymn 2015).
As Douville et al. (2020) suggest, knowledge about how to prevent infection can be just as important as treating an infection once it has already occurred, yet, there are still considerable international variations in terms of the recommended protocols. Advances in wound dressings and surgical techniques to prevent infection is an ongoing area of research, and is yet another aspect of midwifery care that is continually evolving in line with recent medical discoveries (Douville et al. 2020).