Peptic Ulcers: Types, Symptoms and Treatment
Published: 16 November 2022

Published: 16 November 2022

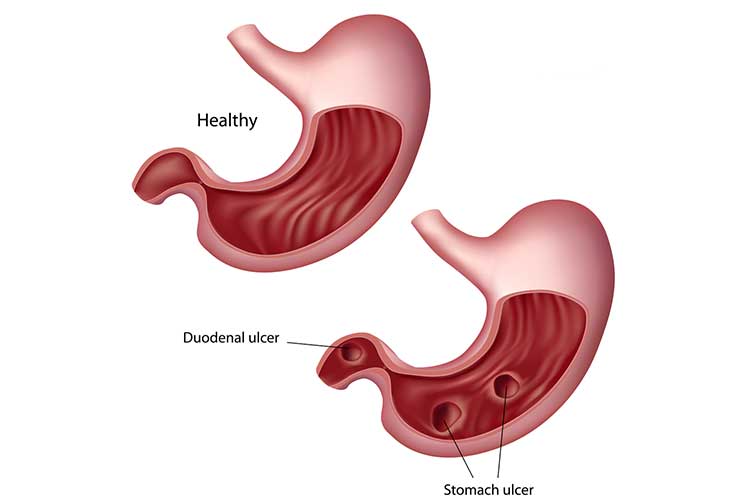
Peptic ulcers occur in the lining of the stomach or on the upper section of the small intestine (duodenum). They can be categorised as either:
(Mayo Clinic 2022; American College of Gastroenterology 2021)
Normally, the lining of the stomach and intestines has defences against acid produced by the stomach. However, when something interferes with those defences, the acid may cause damage. A peptic ulcer is a product of this damage; it is an open and inflamed sore (MSD Manual 2021; Mayo Clinic 2022).
While peptic ulcers are common and treatable, it’s crucial that they are diagnosed early in order to avoid severe complications (MSD Manual 2022; Mayo Clinic 2022).
Ulcers vary in size, ranging from millimetres to centimetres. Peptic ulcers can be differentiated from erosions by the depth of penetration. Erosions are typically more superficial (Vakil 2022).
If left untreated, serious complications may occur.

The most common causes of peptic ulcers are:
(Healthdirect 2021; Mayo Clinic 2022)
Note that spicy foods and stress do not cause peptic ulcers, but can worsen symptoms (Mayo Clinic 2022).
Often - in up to three-quarters of people - peptic ulcers will not present with any symptoms (Mayo Clinic 2022).
If symptoms do occur, they most commonly include a burning or gnawing pain in the upper abdomen. This pain can travel to the chest, neck, belly button or back (Healthdirect 2021). The pain often comes and goes in intervals (Vakil 2022).
Other, less-common symptoms include:
(Healthdirect 2021)
Eating food may dull the symptoms of duodenal ulcers but will often worsen the symptoms of gastric ulcers (Vakil 2022).
Peptic ulcers may lead to the following:
(MSD Manual 2022; Vakil 2022)
Peptic ulcers are common and can affect people of any age. However, they mostly occur in people over 60 and men are more commonly affected than women (NHS 2022).
Previously, stress, diet and smoking were thought to be the leading causes of stomach ulcers. It is now known that H. pylori bacteria are the main cause of ulcers (Queensland Government 2017).
H. pylori infection is present in 50 to 70% of patients with duodenal ulcers and 30 to 50% with gastric ulcers (Vakil 2022).
NSAIDs account for more than 50% of peptic ulcers (Vakil 2022).
Smoking is still considered a risk factor for the development of ulcers and the complications they cause. Additionally, smoking is known to impede healing and increase the chance of recurrence. For children with duodenal ulcers, in 50 to 60% of cases, there is a family history - this is thought to be due to H. pylori being transmitted between family members (Vakil 2022).
Treatment of gastric and duodenal ulcers involves removing the cause, which may require:
(MSD Manual 2022)
A general practitioner may suggest an examination if a person has stomach pain characteristic of ulcers.
Tests are needed to confirm the diagnosis:
(Vakil 2022)
An upper endoscopy is the method most commonly used to diagnose a peptic ulcer, during which, a biopsy looking for H. pylori bacterium or cancer will be taken. This, combined with a patient history, will form the diagnosis (Vakil 2022).

(Mayo Clinic 2022)
Question 1 of 3
Which one of the following is NOT a risk factor for a peptic ulcer?